Feature Story
As published in the UConn Advance, October 6, 2008.
Paper Suggests Patients Supplement Blood Pressure Readings
By Chris DeFrancesco
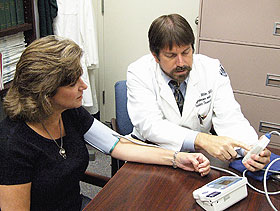
Dr. William White, co-author of an American Society of Hypertension position paper on self-monitoring of blood pressure, demonstrates the use of an ambulatory blood pressure monitor and a home blood pressure monitor.
Photo by Chris DeFrancesco
Having your blood pressure checked in the doctor’s office is not the only way to keep tabs on your hypertension. It may not even be the most precise way.
“Blood pressure readings should be taken both in and outside of the medical care environment,” says Dr. William White, professor of medicine in the Pat and Jim Calhoun Cardiology Center at the UConn Health Center.
“Blood pressure values are highly variable throughout the day and night, so taking one or two measurements during an office visit often doesn’t capture the truth about blood pressure behavior. Additionally, our research over the past two decades has made it clear that monitoring in the office alone isn’t always the most reliable method for assessing blood pressure control in patients on antihypertensive drug therapy.”
White and Dr. Thomas Pickering from Columbia Presbyterian Medical Center in New York City are co-authors of an official American Society of Hypertension position paper on home and ambulatory blood pressure monitoring, published in the May-June 2008 issue of the Journal of the American Society of Hypertension.
The paper provides guidance on when to supplement in-office blood pressure measurements with out-of-office techniques, such as self-monitoring at the home or worksite and ambulatory blood pressure monitoring.
“Self and ambulatory blood pressure monitoring can provide unique information that may be of help both for making treatment decisions and for evaluating the response to treatment,” the authors write.
“The mainstay for the justifications of both procedures is that there is steadily increasing and substantial evidence that both measures give a better prediction of cardiovascular risk than office blood pressure measurements.”
Self-monitoring devices enable patients to take their readings at home at several points throughout the day. Oscillometric blood pressure monitors, which use technology that senses pressure waves emanating from the brachial or radial artery, are available in drug stores and medical supply shops and through catalogs, generally ranging in price from $50 to $150.
Ambulatory blood pressure recording involves wearing a cuff on the upper arm, typically for a 24-hour period. The cuff is attached to a monitoring device clipped to the patient’s belt. A microchip in the monitor stores the data for analysis and display.
The Calhoun Cardiology Center provides 24-hour ambulatory blood pressure monitoring upon referral from the patient’s primary care doctor or medical sub-specialist. White’s research and testimony led to Medicare coverage of ambulatory monitoring tests, starting in 2002.
“Done properly, these methods increase the number of readings used to calculate average blood pressure, and therefore give much better estimates, yielding a better prediction of risk than the office measurement alone,” White says.
He emphasizes that only devices that have been independently validated for precision and reliability should be used for self- or ambulatory monitoring. Physicians and patients can determine grading from independent studies at the Dabl Educational Trust web site: www.dableducation.org
White, head of the Calhoun Cardiology Center’s Hypertension and Clinical Pharmacology Division, says these out-of-office measurements offer another advantage.
“One often hears the term ‘white-coat hypertension’ or ‘white-coat effect’ to describe a phenomenon when the patient’s blood pressure is high in the medical care environment but relatively normal elsewhere,” he says.
“This can be a manifestation of anxiety in the doctor’s office that does not occur anywhere else. However, we also have seen the converse to be true; that is, patients actually have a higher pressure outside of the doctor’s office, particularly when medications are wearing off—a syndrome called ‘masked’ or ‘hidden’ hypertension. This is more problematic, as the doctor assumes the pressure control is acceptable, when actually hypertensive blood pressure values are occurring throughout the day and night – clearly a risk factor for cardiovascular problems, including heart attack, stroke, and kidney disease.”
A call to action by the American Society of Hypertension, the American Heart Association, and the Preventive Cardiovascular Nurses Association recommends that home monitoring become a routine component of blood pressure measurement in the majority of patients with known or suspected hypertension.
It also recommends that health care providers advise patients to use monitors that measure blood pressure on the upper arm and show them how to use the devices. Additionally, it calls for health insurers to reimburse patients who purchase them.


